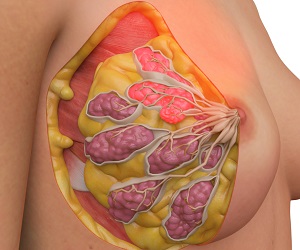
What is Mastitis?
Mastitis is inflammation of the breast tissue in your mammary glands often caused by blocked milk ducts but sometimes involves an infection. The condition most commonly affects women who are breastfeeding (lactating women).
How Does Mastitis Develop?
Mastitis develops when certain bacteria (typically staphylococci or streptococci) from the baby's mouth enters the milk ducts through your breast nipple.
Mastitis can occur with or without infection present.
Mastitis without infection
- This is caused by milk stasis. Here, mastitis occurs when milk builds-up within your breast tissue and is trapped in the breast due to the clogging of milk ducts.
Mastitis with infection
- This is caused by bacteria. Here, the bacteria from your baby’s mouth enters your breast tissue via the cut or cracked nipple and infects the breast tissue to cause inflammation.
Who is at Risk of Mastitis?
You are at increased risk of developing mastitis if you are:
- Breastfeeding with cracked or sore nipples
- Breastfeeding using only one position
- Wearing a bra that is tight-fitting leading to restriction of milk flow
- Having previous episodes of mastitis while breastfeeding
- Feeling extreme tiredness or fatigue or stress
- Using an improper nursing technique
- Poor nutritional intake
In situations like those listed above, there is every possibility of milk build-up within the breasts leading to infection of the breast tissue.
Signs and Symptoms
The most common symptoms of mastitis include:
- Breast tenderness, abnormal swelling, redness and warm to the touch
- Pain or burning sensation in the breast while feeding the baby
- Breast tissue thickening and itching or development of a lump in the breast
- Feeling run down (fatigue, tiredness), chills and illness
- Flu-like body aches and occasionally fever of 101 F (38.3 C) or more
Possible Complications of Mastitis
If mastitis is not treated appropriately and adequately, it may progress and result in a localised collection of pus in your breast tissue (breast abscess). The condition may turn severe and can even be fatal if untreated.
Diagnosis
Mastitis is easy to detect and normally diagnosed clinically (examination of the actual patients). Your doctor will first physically examine the affected area, then ask you a few questions and finally look for symptoms of mastitis. Once confirmed of the condition, the doctor will prescribe treatment.
However, if you do not respond to the initial treatment, your milk sample may be taken to test for other conditions including cancer.
Treatment
Treatment of mastitis depends on the severity of the condition and ranges from antibiotic prescription to minor surgery.
Initially, you will be administered antibiotics intravenously (through veins) or orally (through the mouth) to eradicate the bacterial infection.
Cautionary
Treatment notwithstanding, mastitis can recur during breastfeeding in case you:
- Have sore nipples or plugged ducts
- Have breasts not fully emptied of milk
- Do not finish the antibiotic course for original infection
- Have a history of lumps
- Suffer from low iron (anaemia) or stress
- Wear tight clothing
- Are a smoker
If the condition does not improve despite the treatment, your doctor will recommend a simple surgery that involves “incision and drainage”.
Prognosis
Mastitis symptoms will clear up within a few days if you carefully follow the doctor’s treatment directions and complete the entire prescribed antibiotics course.
Prevention of Mastitis
The following tips can help you to minimize or prevent your chances of getting mastitis:
- Keep your nipples crack free and breastfeed frequently
- Fully drain the milk from your breasts while feeding
- Allow your baby to empty one breast before switching to another
- Change the position of breastfeeding every time
- Allow your baby to latch on properly during feedings
- Quit or stop smoking if you are a smoker
Speak to your doctor before starting breastfeeding so they can provide instructions and tips for successful breastfeeding.
